Diagnosis of oligohydramnios during the second trimester is more likely to be associated with fetal or maternal anomalies, whereas diagnosis in the third trimester is more likely to be of unexplained origin. The management and prognosis of oligohydramnios vary greatly depending on the underlying etiology, the gestational age at diagnosis, and the severity of oligohydramnios. Therefore, fetal gastrointestinal anomalies, such as tracheoesophageal fistula (incidence rate of approximately 1 in 3500 live births), can result in excess fluid volume, or polyhydramnios. Fetal swallowing and intramembranous absorption, thought to occur by osmotic absorption of fluid directly across the amnion and into fetal blood vessels, are the primary routes of amniotic resorption. Examples include bladder outlet obstruction, dysplastic kidneys, and renal agenesis. įetal genitourinary abnormalities can, therefore, result in a diagnosis of oligohydramnios after 16 to 20 weeks gestation. At around week 16, the fetal kidneys begin to function, and the production of fetal urine steadily increases, taking over the majority of amniotic fluid production until the gestation is at term. In the first 20 weeks, lung secretions, along with hydrostatic and osmotic transport of maternal plasma through the fetal membranes, make up the majority of amniotic fluid production. The volume of amniotic fluid in the gestational sac is a result of a balance between fluid production and fluid movement out of the sac. The MVP should serve to evaluate oligohydramnios in multifetal pregnancies, as you will not be able to measure all four quadrants for each fetus. With this in mind, some institutions opt to use the MVP in gestations with low AFV and use the AFI in cases of high AFV. The use of the maximum vertical pocket tends to overly diagnose cases of polyhydramnios, while the use of the AFI tends to underdiagnose cases of oligohydramnios. An AFI <5cm is consistent with oligohydramnios. The sum of the four maximum vertical pockets is equal to the AFI. 
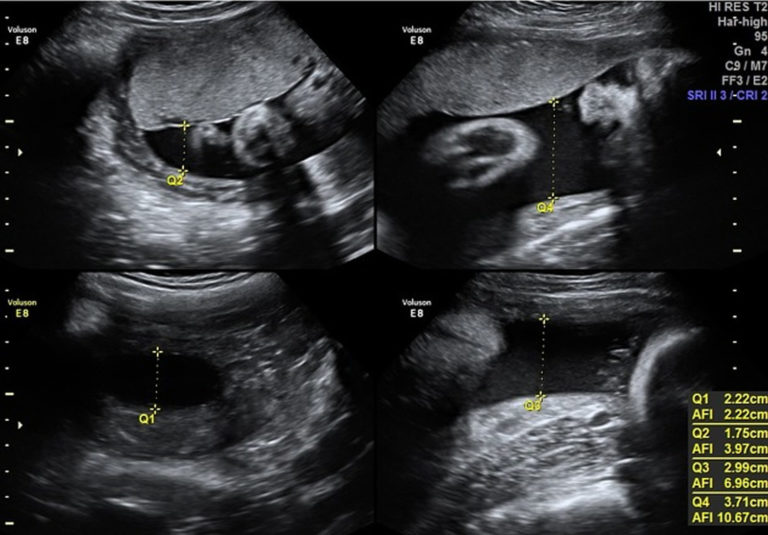
The AFI can be determined after 20 weeks of gestation by dividing the uterus into four quadrants through the umbilicus and determining the MVP in each quadrant. The amniotic fluid index (AFI) is an alternative assessment of AFV. The normal range for MVP is 2-8 cm: a pocket 8 is considered polyhydramnios. 
The measurement should be made from the 12 o’clock position to the 6 o’clock position. The sonographer systematically scans the abdomen and obtains an image that demonstrates the maximum vertical pocket - the deepest pocket of amniotic fluid that does not include fetal umbilical cord or body parts. Transabdominal ultrasound evaluation of AFV includes the use of either the maximum vertical pocket (MVP) or the amniotic fluid index (AFI) depending on the institution. Discrepancies should prompt an amniotic fluid assessment by ultrasound. Īmniotic fluid disorders should be included in the differential diagnosis whenever there is a discrepancy between the fundal height measurement and gestational age. This pattern allows for clinical assessment of AFV throughout pregnancy using fundal height measurements and ultrasound evaluation. The AFV then begins to decrease steadily after 40 weeks gestation, leading to reduced volume in post-term gestations. The volume of amniotic fluid changes over gestation, increasing linearly until 34 to 36 weeks gestation, at which point the AFV levels off (approximately 400mL) and remains constant until term. Oligohydramnios is defined as decreased amniotic fluid volume (AFV) for gestational age. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
